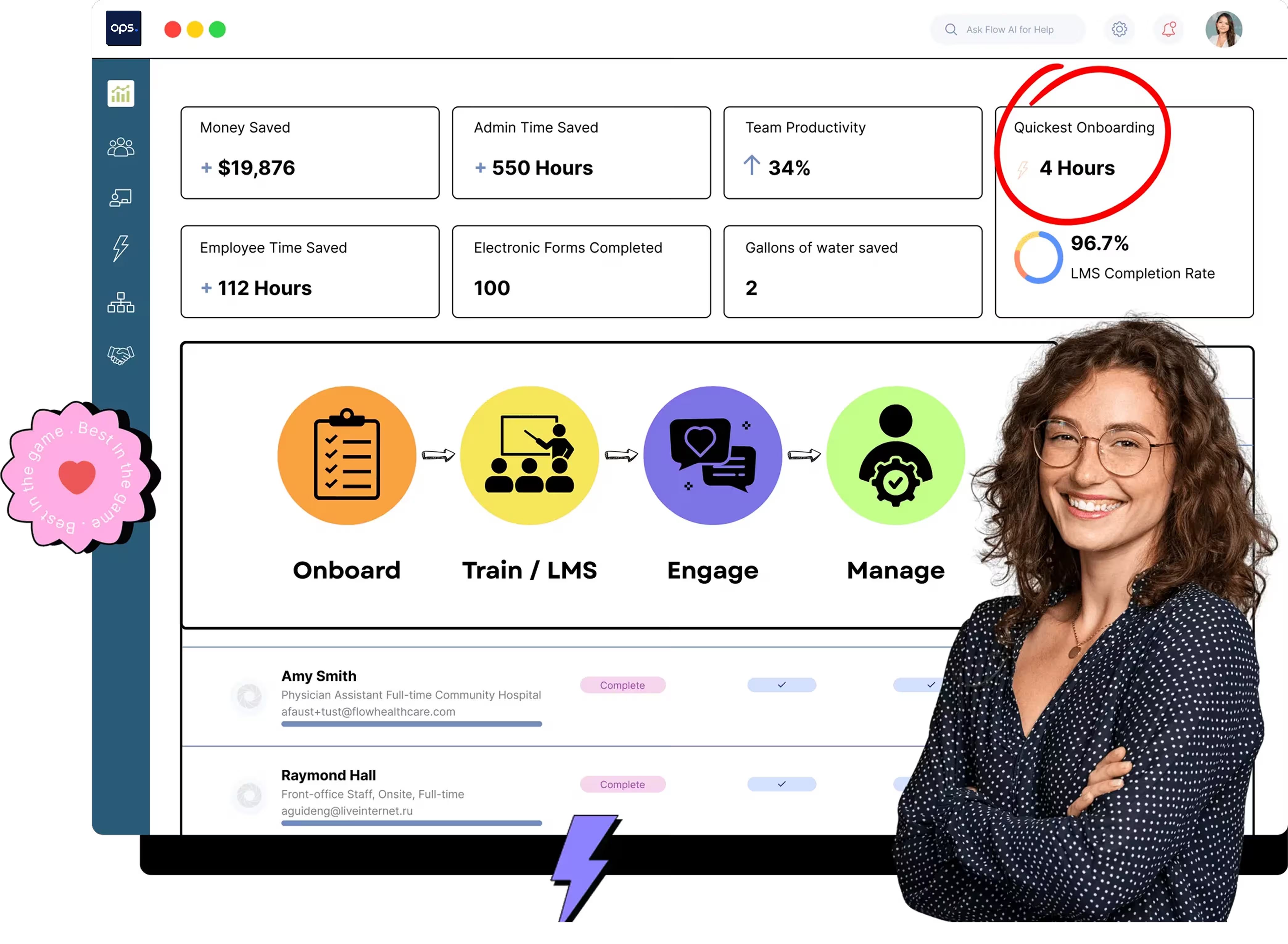
A structured program can halve time-to-productivity and boost first-year retention rates by 82%, saving organizations about $600 per new hire. Poor onboarding contributes to a 25% turnover rate. An effective onboarding checklist should be developed 90 to 45 days prior to the new hire’s start date. A focused onboarding program continues through the first 90 days of employment, and ongoing support is provided well into the first year.
Key Takeaways
- Effective onboarding is key to staff retention
- Onboarding follows a three-phase framework that begins before the new hire’s start date: planning, execution, and management
- Disorganized onboarding contributes to compliance gaps and a 25% first-year turnover rate
- Ongoing education improves patient care and staff retention
- Monitor for signs of employee disengagement or dissatisfaction regularly to prevent turnover
- Successful onboarding results in fully integrated team members contributing to patient care and organizational success
Building cohesive healthcare teams requires systematic integration, not just filling positions. Most healthcare organisations treat the onboarding process as a set of administrative checkboxes rather than a strategic operation.
A structured onboarding program reduces time-to-productivity by 50% and improves first-year retention by 82%. Healthcare organizations save an average of $600 per new employee through administrative efficiency. Disorganized onboarding creates compliance gaps and contributes to 25% first-year turnover rates.
This guide presents a three-phase framework for onboarding new employees. A good onboarding plan establishes clarity, execution transforms paperwork into practice, and management ensures sustained staff and team performance.
A. PLAN: What Should You Include in a Healthcare Onboarding Checklist?
Start 90 To 45 Days Before the Target Start Date
Effective onboarding in healthcare begins long before the first shift. Onboarding planning establishes role clarity, maps dependencies, and coordinates resources.
Done well, planning eliminates 80% of common onboarding delays and ensures compliance. Done poorly, it guarantees a poor healthcare onboarding experience for all parties involved.
1. Define Role Requirements with Precision (3 - 5 hours)
Vague job descriptions create mismatched expectations and onboarding chaos. Document exactly what success looks like before posting positions.
Step 1: Clarify the Clinical Context
Different healthcare settings demand different capabilities. An emergency department nurse requires different skills than an ambulatory surgery nurse practitioner.
A respiratory therapist in the NICU needs different expertise than one in pulmonary rehabilitation. Medical assistants in primary care follow different workflows than those in orthopedic surgery.
- Define the specifics of each healthcare environment. Identify the department, unit, or clinic location clearly.
- Specify patient population: pediatric, geriatric, surgical, or behavioral health. Clarify the care model: inpatient, outpatient, procedural, or consultative.
- Document physical demands and safety considerations for the role.
Step 2: Map Daily Responsibilities for all Clinical Staff
Detail the typical workday in concrete terms. Include shift structure and hours.
Specify patient volume or procedure counts per shift. Identify team composition and who they work alongside daily.
List the equipment and technology used regularly. Document administrative or documentation requirements.
Example: Surgical technicians in orthopedics handle 4-6 cases daily with significant physical demands. Cardiac cath lab techs manage 8-12 shorter procedures with different equipment.
Step 3: Identify Required Credentials
Separate mandatory requirements from preferred qualifications clearly.
Mandatory requirements include active professional licenses. These cover RN, LPN, CNA, RT, and ARRT credentials.
Required certifications include BLS, ACLS, and specialty credentials. Immunization compliance and health clearances are non-negotiable.
Background check and drug screening standards must be met.
Preferred qualifications include years of experience in similar settings. Familiarity with various Electronic Health Records (EHR) platforms provides added value.
Specialty certifications or advanced training are beneficial. Bilingual capabilities contribute to high-quality care.
Step 4: Choose the Employment Model
Most healthcare roles operate as W-2 employment. This provides benefits and payroll tax coverage.
Full organizational integration comes with W-2 status. Some organizations utilize per diem arrangements for scheduling flexibility.
Contract healthcare staffing provides temporary coverage when needed. Each model affects administrative requirements and how comprehensive onboarding is.
Step 5: Create the Role Summary
Consolidate everything into a one-page document. Include the position title and department clearly.
Specify FTE or hours per week commitment: detail shift patterns and weekend requirements.
Document reporting structure for clinical staff and administrative roles. List required licenses and certifications.
Outline core responsibilities with the top 5-7 duties. Include the target start date and compensation range.
Distribute this summary to all stakeholders. Healthcare HR, department managers, credentialing staff, and training coordinators need copies.
IT support should receive the summary as well. It becomes the master reference throughout the hiring and onboarding processes.
2. Map Timeline Dependencies (2–3 hours)
Most onboarding delays stem from unrecognized dependencies. Background checks take longer than expected.
Occupational health appointments fill weeks in advance. License verifications drag through the state bureaucracy.
Identifying dependencies upfront transforms uncertainty into manageable timelines and creates a better onboarding experience for medical staff.
Critical Timeline Elements:
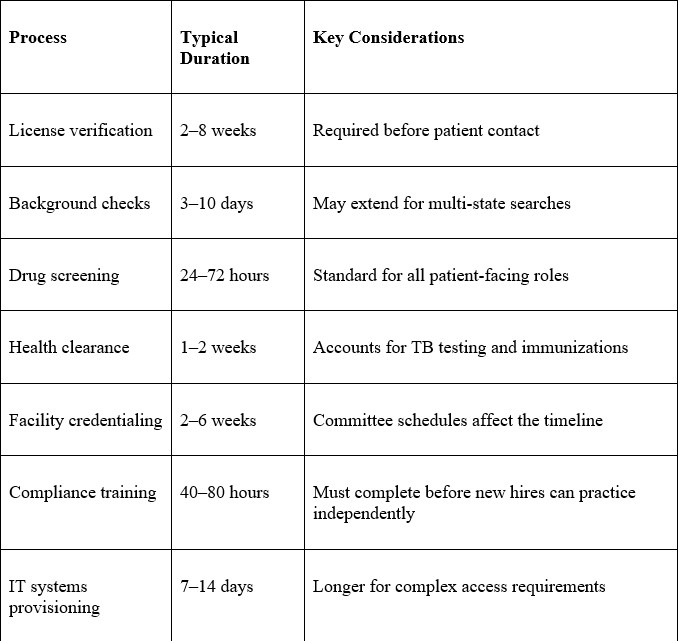
Work backwards from your target start date. If the onboarding process begins September 1, initiate license verifications by early July.
Submit background checks by mid-August. Request IT access no later than mid-August.
Build a Visual Timeline:
Create a tracking system showing the start date as an anchor. List each dependency with the owner and due date.
Use status indicators: Not Started, In Progress, Complete, or Blocked. Maintain a weekly update cadence, keeping stakeholders aligned.
Modern healthcare onboarding software automates much of this coordination. Systems trigger sequential steps as prerequisites are completed.
This reduces manual tracking burden by 50%.
3. Assemble Complete Documentation (8-15 hours)
Incomplete credentialing packets cause more delays than any other factor. Build comprehensive documentation upfront and store it centrally.
All internal teams can then access verified information.
Essential Documents:
- A current resume with complete work history is required. Active professional licenses with expiration dates must be included.
- All required certifications need documentation: BLS, ACLS, PALS, and specialty credentials. Education verification through transcripts or diplomas is mandatory for all healthcare professionals.
- Government-issued photo ID and Social Security documentation are necessary. Complete immunization records must cover MMR, varicella, Tdap, hepatitis B, TB testing, and flu.
- Physical examination and health clearance from approved healthcare providers. Background check authorization and results must be current.
- Drug screening consent and results are required. Professional references need verification - minimum three with confirmed contact information.
- Previous employment verification is essential. National Provider Identifier applies to billing roles.
Acceleration Strategies:
- Request documentation immediately upon offer acceptance. Don't wait until the start date to begin collection.
- Use digital platforms enabling secure document uploads. Credentialing staff, HR, and compliance teams access the same verified information simultaneously.
Ops.work's platform addresses this challenge directly. Electronic document management includes autofill technology that reduces completion time.
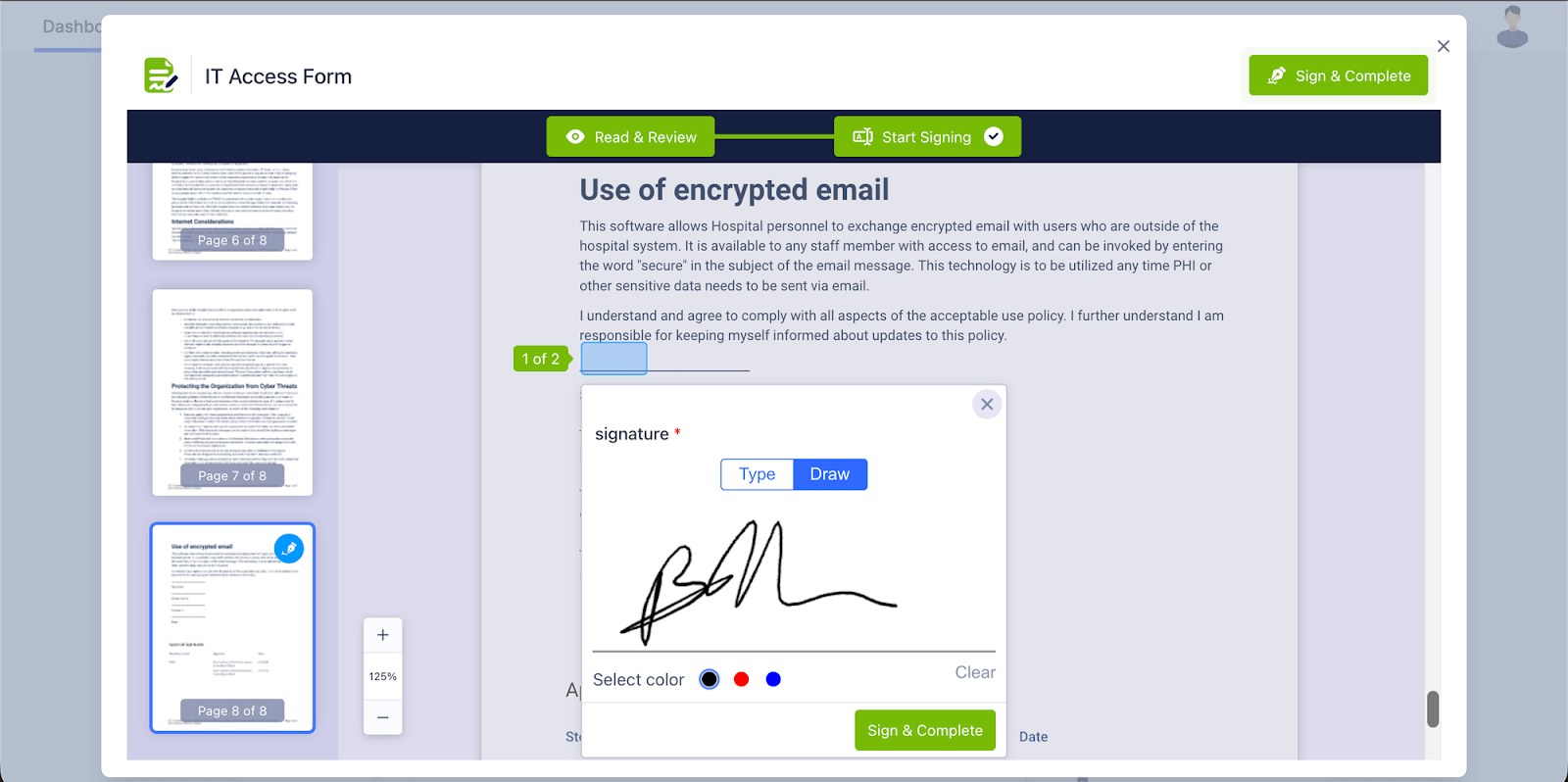
Electronic signatures eliminate printing and scanning delays. Centralized storage prevents duplicate requests from different departments.
4. Coordinate Systems Access (2-4 hours)
Technology access problems are the most common Day One complaint. Newly hired employees can't log into email or access the EHR.
They can't badge into their unit upon arrival. These delays are entirely preventable with advance planning.
IT departments typically require 7-14 days to provision accounts. Submit comprehensive access requests when background checks are clear.
An email account with calendar functionality is essential. EHR system login needs role-appropriate permissions.
Access to the time and attendance system is required. Department communication tools include secure messaging and coordination platforms.
Building access credentials and ID badges must be ready. Phone or paging systems apply when needed.
VPN enables remote access when required.
Create standardized access templates by role type. When hiring a medical assistant, automatically request the standard medical assistant access package.
Hospital staff onboarding automation platforms reduces IT coordination time by 70%. This templated approach eliminates repetitive manual work.
5. Design Training Pathways (5–10 hours)
Generic orientation fails because it ignores role-specific learning needs. Effective onboarding training operates in three distinct tiers.
Universal Training applies to all employees regardless of role. This covers organizational mission, values, and culture.
Compliance fundamentals include HIPAA, OSHA, and infection control. Emergency procedures and safety protocols are essential.
Facility geography and key resources get covered here.
Department-Specific Training tailors content to the work environment. Unit workflows and communication patterns are taught.
Documentation standards and templates are explained. Equipment operation and maintenance receive attention.
Patient population characteristics are described in detail.
Role-Based Competencies validate technical skills through hands-on demonstration. Supervised practice includes immediate feedback.
Formal sign-off confirms capability before independent work.
A healthcare training management system automates assignments based on position. Location and employment status determine the specific modules assigned.
When a phlebotomist joins the lab, universal compliance training is assigned automatically. Laboratory department modules and phlebotomy competency validations follow.
No manual coordination is required at all.
Ops.work enables this capability through drag-and-drop workflow creation, auto-assignment works based on role and location.
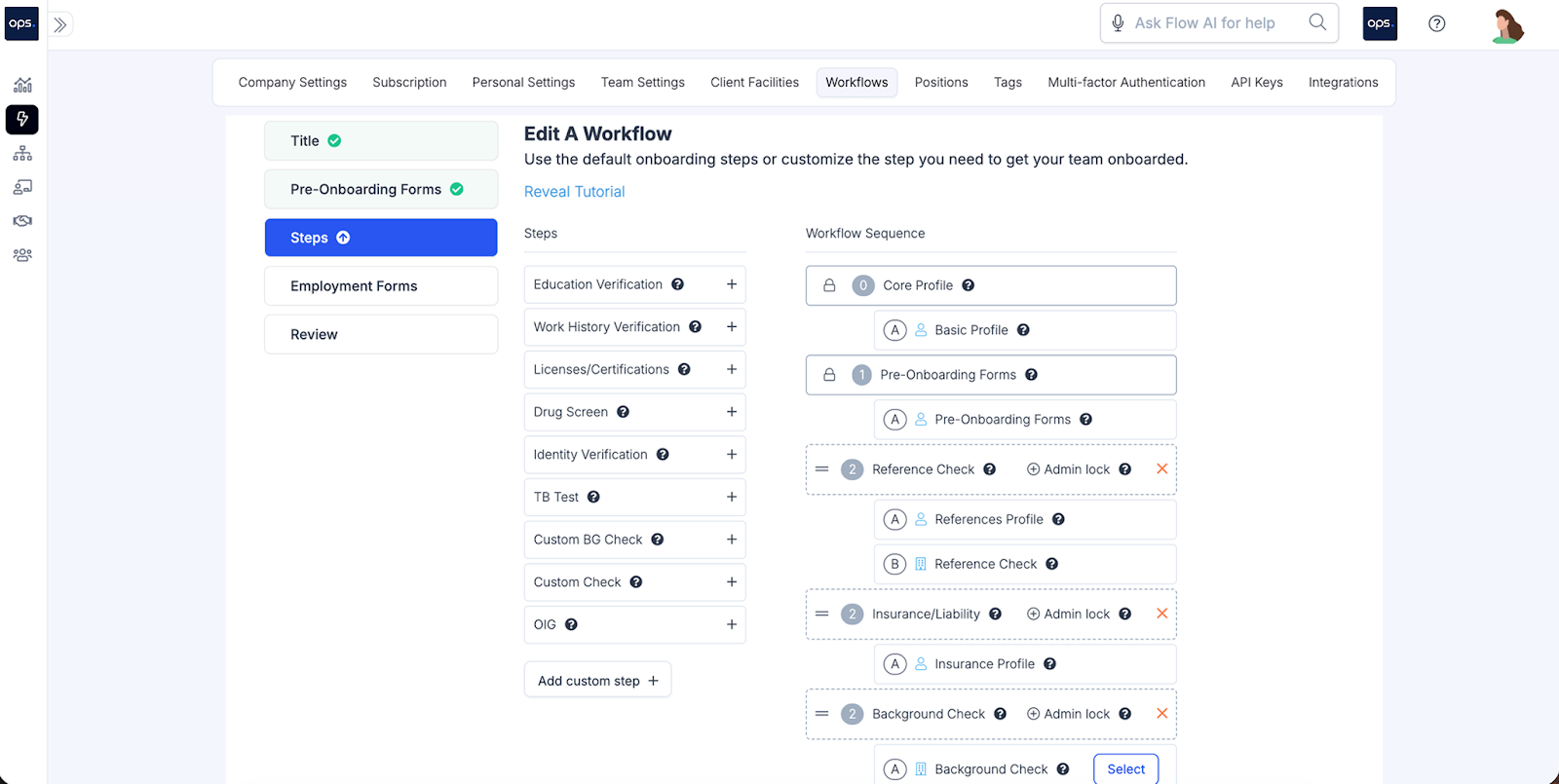
This eliminates missed training materials discovered weeks after the start date.
6. Prepare the Welcome Experience (1-2 hours)
Healthcare organizations with structured orientation programs see 34% higher engagement at 90 days. Ad hoc approaches produce significantly lower results.
First impressions shape retention significantly. A chaotic first day signals disorganization and bad onboarding.
A structured welcome signals professionalism and respect.
Pre-Arrival Communication should be sent one week before the start. Include arrival logistics: parking, entrance, and who to ask for.
Specify dress code and what to bring. Provide first-week agenda overview.
List key contacts with phone numbers. Include any required pre-work with access instructions.
Day One Logistics must be ready in advance. Workspace or locker assignment should be prepared.
ID badge should be ready for pickup. Computer credentials should be provided in writing.
The training schedule needs confirmation before arrival. Mentor or buddy gets introduced immediately.
Lunch arrangements matter, never leave new hires alone on Day One.
7. Budget for True Costs (1-2 hours)
Understanding actual onboarding costs enables ROI calculation. This justifies process improvements and technology investments to healthcare leaders.
Typical Cost Per Hire:
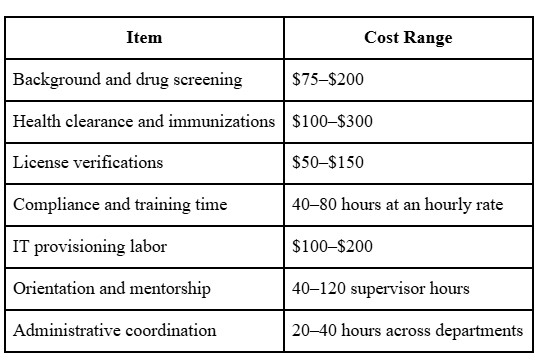
Total onboarding cost typically ranges from $3,000 to $8,000 per hire. Role complexity and organizational efficiency affect final numbers.
By the end of the planning phase, your healthcare onboarding checklist should include:
- Role requirements are documented and distributed to all stakeholders.
- Timelines with dependencies are mapped and tracked actively.
- The complete credentialing packet is assembled and verified.
- IT access requests have been submitted on time.
- Training pathways are designed and scheduled appropriately.
- Welcome communication is prepared and ready to send.
- Budget tracking is established for cost monitoring.
B. EXECUTE: What are Healthcare Onboarding Best Practices for Implementing Your Onboarding Checklist?
From 45 Days Before Start to 30 Days After Start
An exceptional onboarding process includes execution, which transforms planning into action. Credentials get verified, and training is deployed.
Systems activate, and new team members transition to active status. This phase requires precision and rapid problem-solving.
1. Verify Licenses and Certifications (2-8 weeks, 4-10 admin hours)
Healthcare onboarding must include license verification for clinical roles to ensure quality care from day one. The timeline varies by state and credential type.
License Verification Process:
Submit a verification request to the state licensing board immediately. Provide notarized authorization if required by the state.
Track status weekly and escalate any delays promptly. Confirm active, unencumbered status before proceeding further.
Timeline expectations vary significantly by situation. In-state verification typically takes 1-3 weeks.
Out-of-state verification requires 2–6 weeks, typically. Compact license verification completes in 1-2 weeks.
Certification Verification:
Confirm current status for BLS, ACLS, PALS, and specialty credentials. Verification happens through issuing organizations directly.
Check expiration dates carefully and thoroughly. Ensure credentials extend at least 90 days past the start date.
Schedule renewals immediately if expiring soon.
Common delays include name discrepancies on documents. Lapsed continuing education credits create problems, too.
Disciplinary actions require explanation and documentation. Address these proactively rather than discovering them late.
2. Process Background Checks and Health Screenings (3-10 days, 1-2 admin hours)
All patient-facing healthcare employees require comprehensive background screening. This includes national criminal database searches and county-level criminal history.
Sex offender registry checks are mandatory for all. OIG/GSA exclusion list verification confirms Medicare/Medicaid eligibility.
Traditional background check processes involve multiple vendor contacts. Manual form submission creates delays and errors.
Modern healthcare onboarding platforms integrate background screening directly. This streamlines onboarding workflows significantly and eliminates redundant steps.
Ops.work enables comprehensive federal, local, and healthcare-level background checks. Processing happens in minutes rather than days.
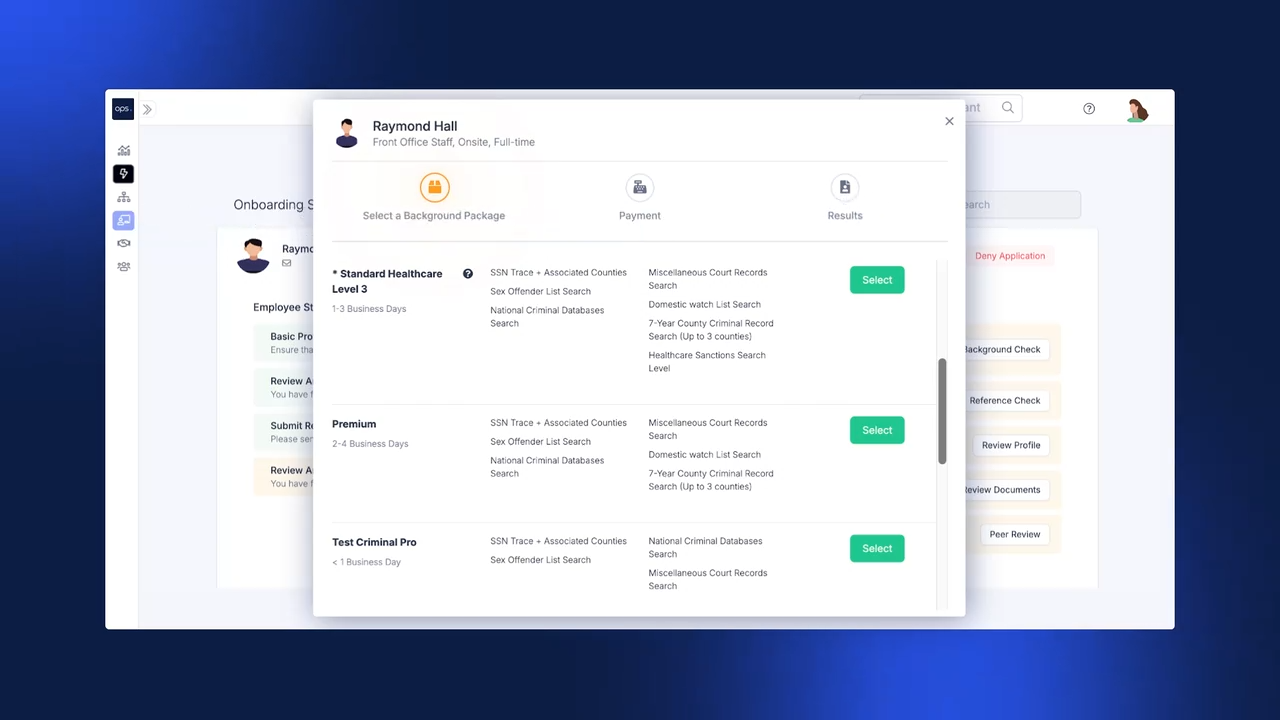
This acceleration during onboarding reduces time-to-start for new hires significantly.
Health Clearance Requirements:
Two-step TB testing applies to all new hires. Immunization verification covers MMR, varicella, Tdap, and hepatitis B.
An annual flu vaccine is required if onboarding during flu season. COVID-19 vaccination follows the current facility policy.
Physical exam and fitness-for-duty clearance are mandatory.
Direct candidates to occupational health immediately upon offer acceptance. Waiting until the week before the start guarantees delays.
This pushes back start dates unnecessarily.
3. Complete Facility Credentialing (2-6 weeks, 8-15 admin hours)
Facility credentialing formalizes authorization to work within the organization. The process includes primary source verification of all credentials.
Licenses, certifications, and references all require verification. Internal compliance review and approval follow verification.
The timeline varies by facility size and complexity. Small clinics complete credentialing in 2-3 weeks.
Community hospitals typically require 3-4 weeks. Large healthcare organizations usually need 4-6 weeks.
Don't wait for final credentialing approval to schedule orientation. Begin training and orientation scheduling during the review stage.
This parallel processing prevents unnecessary delays significantly.
4. Deploy Compliance Training (40-80 hours over first two weeks)
Mandatory compliance training ensures new hires understand healthcare regulations such as HIPAA and OSHA. Infection control and fire safety are included.
Workplace violence prevention is legally required. Emergency procedures and hazardous materials handling are essential.
Every module is legally required and subject to audit.
Best Practices for onboarding training:
Assign training during pre-start onboarding when possible. Pay employees at their hourly rate for completion.
This allows Day One to focus on introductions. Department orientation becomes the priority rather than online modules.
Use auto-assignment based on role and location parameters. A respiratory therapist receives different training from a unit coordinator.
A behavioral health nurse receives different modules than a medical-surgical nurse.
Track completion daily with automated reminders for incomplete modules. Ops.work creates training modules that auto-assign based on position.
Location and employment status determine specific assignments.
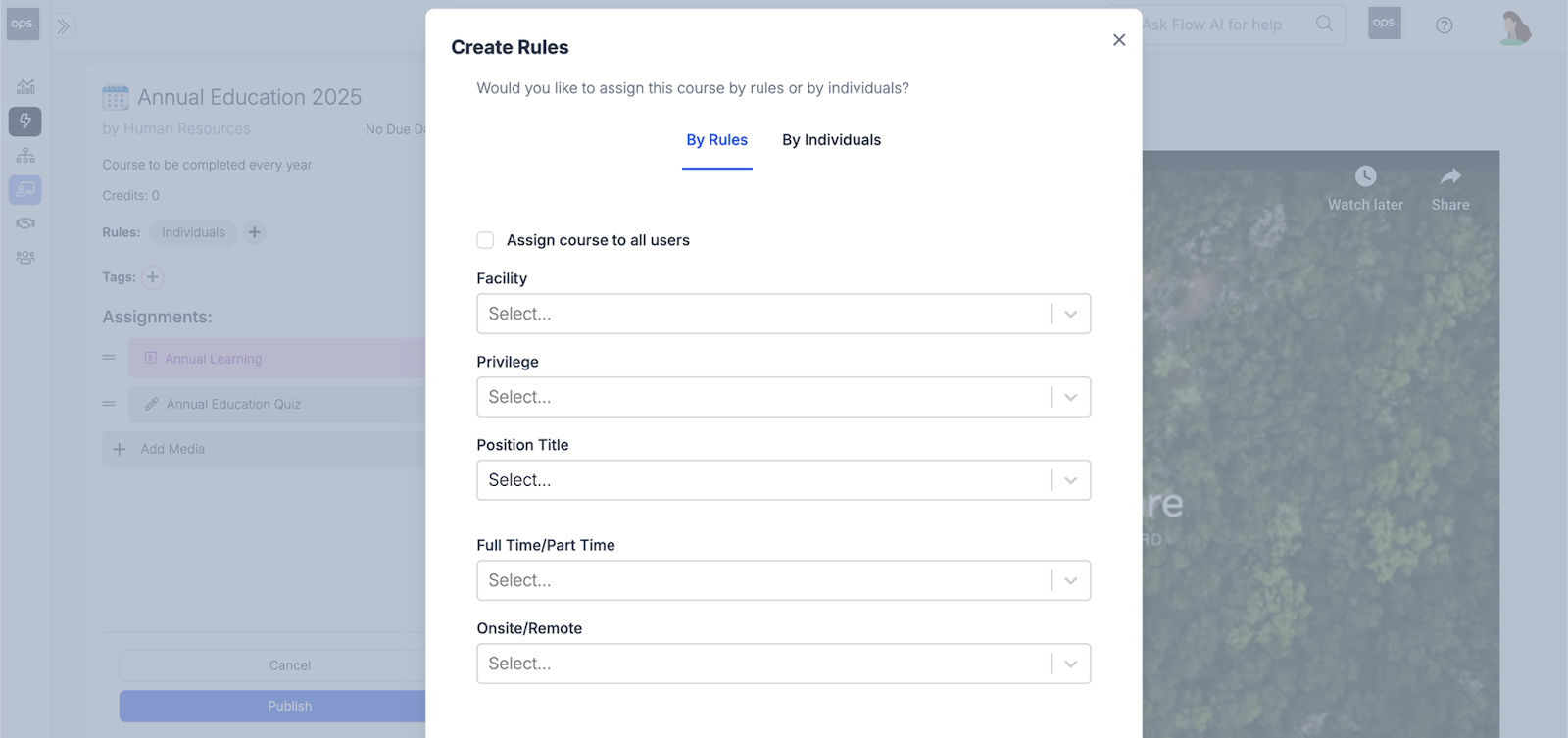
Automatic reminders go to employees who haven't completed requirements.
Ensure all training certificates are uploaded to compliance tracking systems. This provides documentation for audit purposes.
5. Activate EHR and Technology Systems (8-24 hours over the first two weeks)
EHR proficiency determines early productivity more than anything else. Undertrained staff create documentation backlogs and make costly errors.
They experience intense frustration that affects morale.
Training Progression:
Level 1 covers basic navigation during Days 1-2. This includes logging in and finding patients.
Accessing modules and basic menu navigation are taught.
Level 2 addresses core workflows during Days 3-5. Documentation entry and order placement are practiced.
Result review and communication tools are explained.
Level 3 introduces role-specific features during Week 2. Specialized templates and department order sets are demonstrated.
Efficiency tools and shortcuts are taught systematically.
Level 4 covers advanced optimization during Weeks 3-4. Favorites configuration and macros are explained.
Personalized shortcuts and workflows are customized individually.
Combine online modules with hands-on practice in test environments. Include shadowing of experienced users for real-world context.
Require minimum competency demonstration before independent documentation begins.
Pair new hires with EHR "super users" in their departments. These experts provide real-time guidance when questions arise.
This peer coaching accelerates proficiency more effectively than additional modules.
6. Guide Department Integration (First 30 days)
The first month determines whether new healthcare employees feel welcomed or abandoned. Structured progression makes a critical difference.
Week One: Observation and Orientation
Begin with a facility tour and team introductions. Include shadowing without patient care responsibility initially.
Focus on learning physical layout and supply locations. Communication norms and department culture get absorbed naturally.
Week Two: Supervised Practice
Transition to taking on a partial workload with direct supervision. Practice workflows and documentation under guidance.
Receive immediate feedback and coaching on performance. Build confidence through supported skill applications to help new staff provide exceptional care experiences.
Weeks Three–Four: Progressive Independence
Gradually assume full workload with decreasing supervision. Mentors remain available for questions, but are not constantly present.
First formal check-in with the manager addresses any concerns. Adjustments are made based on feedback received.
Assign a dedicated mentor for the first 90 days. Choose experienced, patient staff members to help new hires adjust.
Ensure mentors have protected time to provide adequate support.
End-of-Execution Milestones:
By Day 30, confirm all credentials are verified and active. Background and health clearances must be complete and documented.
Compliance training is finished with all certificates appropriately stored. EHR access is live with basic proficiency demonstrated.
Department orientation is complete with positive feedback received. Mentor relationships are established and functioning well.
The first performance check-in has been conducted thoroughly.
C. MANAGE: How Do You Reduce Staff Turnover with Healthcare Onboarding Best Practices?
From Day 30 to Year 1 and Beyond
The onboarding process doesn't end when training ends, and systems go live. Management is the part of onboarding that transforms new hires into fully integrated team members.
Performance optimization, continuous development, and retention focus drive this phase.
1. Track Performance and Competency (First 90 days, then quarterly)
Conduct well-structured check-ins at 30, 60, and 90 days. Address performance, skill development, team integration, and cultural alignment.
Key Metrics to Monitor:
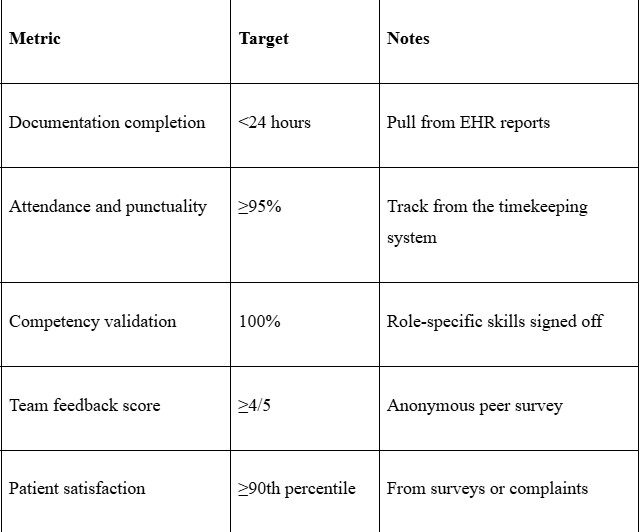
Document specific examples in feedback conversations clearly. "Needs to improve communication" provides no actionable guidance whatsoever.
"On three occasions, critical information wasn't communicated during shift handoff," identifies the issue. This enables targeted improvement efforts.
2. Maintain Compliance and Credentials (Continuous)
Healthcare credentials don't remain valid indefinitely without renewal. A single missed expiration can pull employees off schedule.
This creates compliance violations, operational disruptions, and risks to patient safety.
Renewal Tracking Requirements:
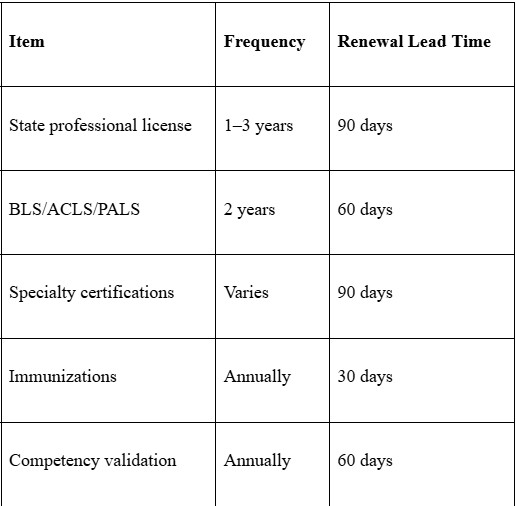
Create a compliance calendar with automated reminders scheduled appropriately. Set alerts at 90, 60, and 30 days before expiration.
Assign clear responsibility for renewal initiation between employees and managers. HR should have oversight of the entire process.
Modern healthcare software automates this tracking completely and reliably. Renewal reminders are sent automatically to the appropriate parties.
Escalation occurs when deadlines approach without action taken. This eliminates discovering expired credentials only during audits or incidents.
3. Support Continuous Development (Month 3 onward)
The healthcare industry requires ongoing education just to maintain current capability, improve patient care, and ensure better patient outcomes. Additional development enables career advancement and staff retention.
Provide clear growth pathways for all team members.
Specialty certification pursuit includes CCRN, CEN, and CNOR credentials. Leadership opportunities involve committee chairs and mentorship roles.
Cross-training in different units or specialties expands capabilities. Educational advancement supports degree completion and advanced training.
High performers appreciate development opportunities and demonstrate higher retention. Many healthcare organizations that invest in growth retain talent more successfully.
4. Identify and Address Retention Risks (6- and 12-month checkpoints)
Turnover costs 1.5 to 2 times annual salary for replacements. This includes recruiting, employee onboarding, productivity loss, and vacancy coverage.
Early identification of turnover risks enables effective intervention.
Warning Signs:
Increased absenteeism or schedule changes signal potential problems. Declining documentation quality or timeliness raises concerns.
Withdrawal from team activities indicates disengagement developing. Visible frustration or conflict suggests dissatisfaction growing.
When patterns appear, conduct immediate "stay interviews" with employees. Ask what's working well and what's frustrating them.
Inquire what would improve the situation meaningfully. Ask what might cause them to consider leaving.
These conversations often reveal solvable problems like scheduling conflicts. Unclear expectations and insufficient resources are common issues.
Feeling undervalued drives many departure decisions unnecessarily. Addressing issues at this stage frequently preserves valuable employees.
5. Calculate Return on Investment (Quarterly)
Executive support for improved healthcare onboarding processes requires demonstrating financial impact. Track specific metrics that quantify value delivered.
Key metrics include time from offer to first productive shift. Administrative hours required per new hire indicate efficiency levels.
First-year retention rate predicts long-term stability and success. Onboarding cost per hire identifies areas for improvement.
Training completion rate and timeline show process effectiveness.
Organizations implementing comprehensive healthcare onboarding software document significant returns consistently. Saving 15 administrative hours per hire at $25/hour equals $375 per person.
For facilities onboarding 100 employees annually, that's $37,500 in labour savings. Countless hours of freed capacity enable higher-value work.
Ops.work documents case studies showing $600 savings per new employee. Administrative onboarding time is reduced by 50% through automation.
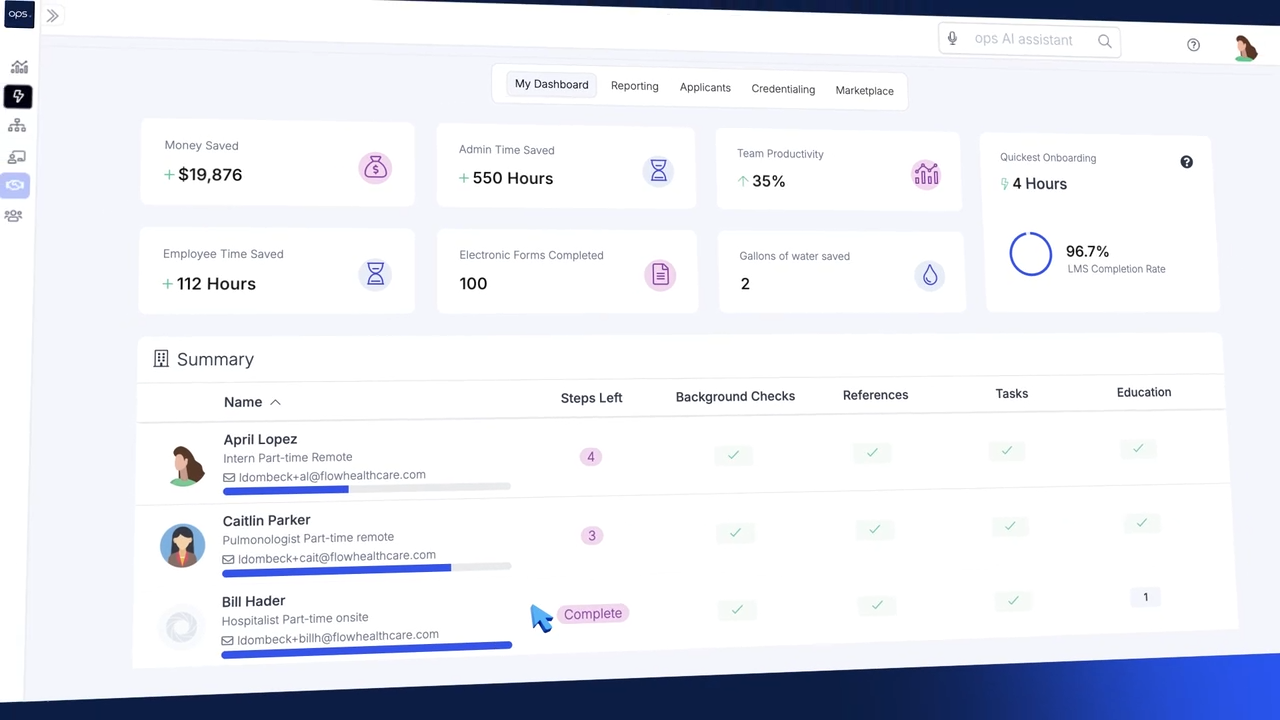
Background checks, reference verification, and document management all streamline significantly. Training assignment automation eliminates manual coordination.
6. Build Continuous Improvement (Ongoing)
Schedule quarterly reviews to examine metrics and gather thorough feedback. Include recent hires and managers in assessment processes.
Identify improvement opportunities based on data and experiences.
Common improvement initiatives include automating manual processes that consume administrative time. Standardizing communication templates creates consistency across all departments.
Enhancing training addresses knowledge gaps identified in performance reviews. Streamlining credential verification happens through better vendor partnerships.
Improving welcome experiences affects first impressions and early engagement.
Each improvement compounds over time and creates cumulative benefits. An initiative saving 30 minutes per hire saves 50 hours annually.
This applies to healthcare organizations onboarding 100 people yearly. Hours are redirected from administrative coordination to employee coaching and development.
End-of-Management Milestones:
By the end of Year 1, confirm all items below. Performance and competency data should be complete and documented.
All credentials must be current with the tracking system active. Professional development opportunities should have been provided to staff.
Positive team feedback and cultural integration should be demonstrated. ROI metrics should demonstrate process efficiency and value.
Continuous improvement initiatives should be identified and prioritized.
At this point, the healthcare team onboarding is complete and successful. The new hire has transformed into a fully integrated team member.
They contribute to patient care and organizational success daily.
Conclusion
Systematic healthcare onboarding represents a competitive advantage in today's environment. Investing in clarity, automation, and structured support transforms your healthcare onboarding significantly.
Technology eliminates most administrative burdens through comprehensive platforms and automation. Automated background checks, streamlined reference verification, and electronic document management reduce coordination time dramatically.
But technology alone doesn't create positive onboarding experiences for employees. Technology enables efficiency while humans create the essential connection and support.
The combination of automated processes and intentional support produces lasting results. Structured check-ins, dedicated mentors, and responsive management boost engagement and retention.
Great healthcare teams aren't found—they're built through purposeful, systematic integration. Onboarding is where that building begins. Try ops.work’s free plan to optimize your onboarding process.
References
Nagib, Nicole, et al. “Onboarding and Early Employment Experiences in Healthcare: Implications for Retention.” Health Services Management Research, 18 Oct. 2025, https://doi.org/10.1177/09514848251384273.
Mosquera, Pilar, and Maria Eduarda Soares. “Onboarding: A Key to Employee Retention and Workplace Well-Being.” Review of Managerial Science, vol. 1, no. 1, 25 Feb. 2025, link.springer.com/article/10.1007/s11846-025-00864-3, https://doi.org/10.1007/s11846-025-00864-3.
Pinco, Ory, et al. “The Onboarding Process: A Review.” Vilakshan - XIMB Journal of Management, vol. 22, no. 1, 18 July 2024, https://doi.org/10.1108/xjm-01-2024-0008.