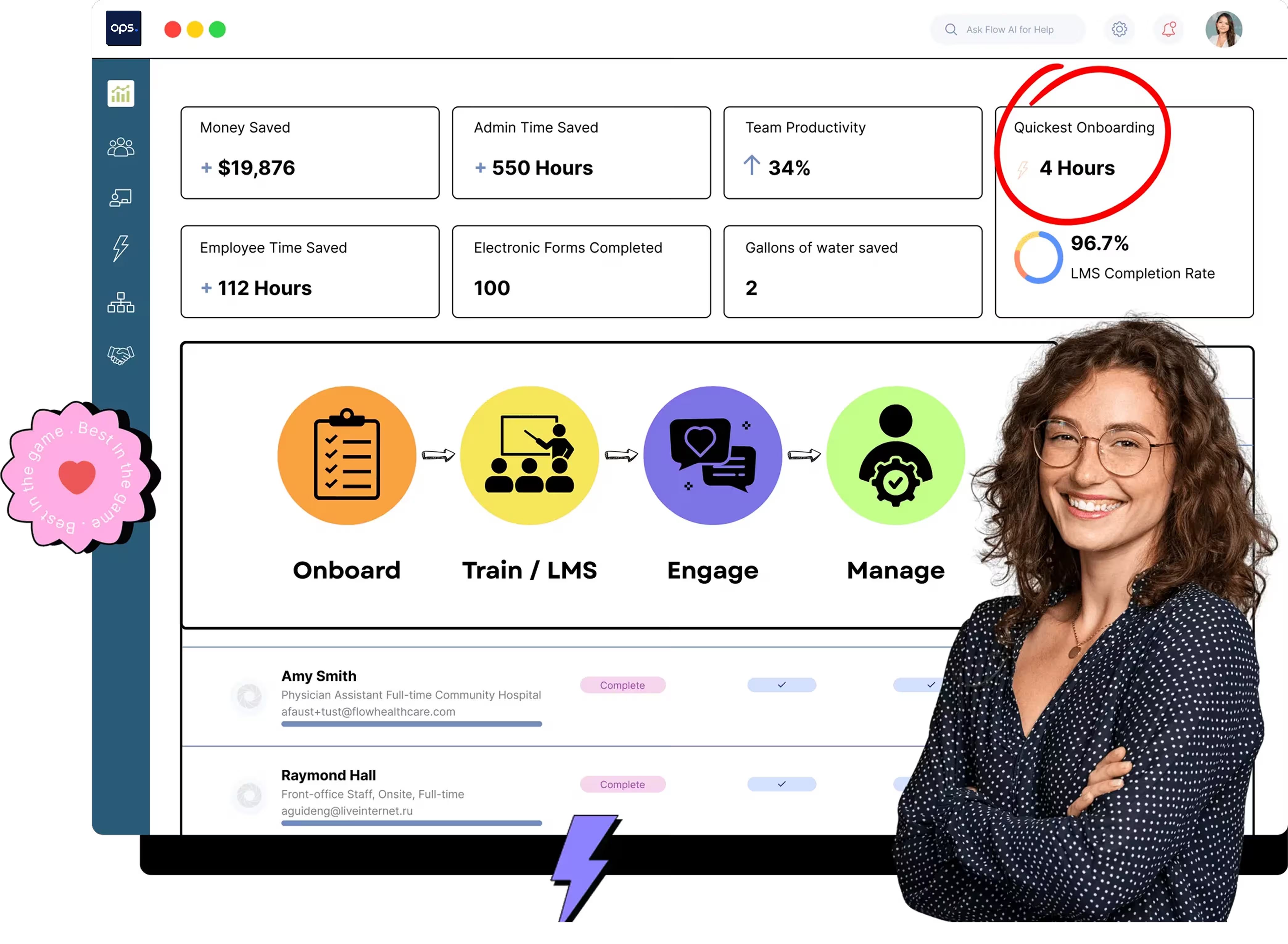
Physician onboarding is a structured, months-long process that integrates new doctors into a healthcare facility, starting before their first day and continuing into their first year. Key stages include credentialing, preboarding, orientation, training, and continuous development. Effective onboarding improves retention, productivity, engagement, and patient outcomes while reducing burnout. A clear checklist and use of technology help streamline tasks, ensure compliance, and support physicians’ long-term success and professional growth.
Key Takeaways
- Physician onboarding equips new physicians with the skills, knowledge and attitudes necessary to provide quality patient care
- Onboarding improves retention, productivity, patient care, and engagement
- Healthcare facilities must verify physician credentials to determine the kind of services they can provide and bill for
- Stages of the physician onboarding process include preboarding, orientation, training, and continuous development
- An onboarding checklist covers the administrative, operational relational, and IT tasks related to integrating new physicians
- Technology tools like ops.work streamline the onboarding process making it efficient
Primary care doctors (MD/DO) are medical professionals who diagnose, treat, and prevent a wide range of medical conditions across all ages. Integrating them into your facility is a months-long process that begins long before they report for their first day and may continue up to the first year of employment. Developing a comprehensive onboarding plan ensures an organized, fulfilling experience, leading to greater job satisfaction and a smoother transition to full clinical duties.
What is Physician Onboarding and Why is it Important?
Physician onboarding is the process of integrating new physicians into a medical facility by providing them with the knowledge, skills, tools, resources, and cultural awareness they need to become productive.
The aim is to support new physicians as they adjust to the new environment, facilitate interpersonal relationships with colleagues, and lay the groundwork for professional development.
Done well, it results in positive experiences for new physicians, resulting in benefits such as:
- Increased physician retention rates
- Higher levels of productivity and performance
- Reduced levels of physician burnout
- Higher patient care quality and better patient care outcomes
- Improved employee engagement rates
What are the Stages of the Physician Onboarding Process?
Effective physician onboarding begins a few months before the official start date to accommodate time and resource-intensive activities such as credentialing. It continues for at least the first 90 days on the job, allowing new hires to acclimate to the new work environment and become productive.
Here are the key stages of a good onboarding program:
Credentialing
Credentialing is the first stage of onboarding physicians. It involves verifying that new hires have the education, licensing, residency, and experience required to provide a certain level of patient care.
It is a mandatory process that ensures healthcare facilities comply with federal, state, and professional requirements when hiring physicians. The credentials a primary care physician requires include:
- An MD or DO degree
- A valid residency program
- Valid State license
- NPI
- DEA license
- Training and safety certifications such as ACLS and BLS
- Malpractice insurance
- CME attestation
- ECFMG certification (for foreign physicians)
- Reference information
- Work experience
- Criminal background checks
Credentialing begins with an application process in which the physician submits all necessary documents and information. Once the physician submits this information, your facility begins the primary source verification (PSV).
PSV involves contacting educational institutions, licensing boards, past employers, malpractice insurance issuers, and governmental agencies, such as the Office of the Inspector General, to verify the validity of the information a physician presented.
Primary source verification is time and labor-intensive, therefore, it should begin as early as possible to avoid delays. Tools such as ops.work streamline the credentialing process, allowing you to collect and verify physician credentials fast.
The next step involves an organizational committee of key stakeholders reviewing the verified credentials to ensure the physician is suited to work in the facility.
If determined suitable, the physician is allowed a range of privileges that determine their scope of practice. They are also enrolled with relevant payers to allow billing for physician services.
After this process, the organization continues to monitor physician credentials to ensure ongoing eligibility to care for patients.
Preboarding
The focus on credentialing may draw attention away from keeping the physician engaged before they report for their first day. The goal of the preboarding phase is to keep physicians engaged and informed as they prepare to begin working at your facility.
This stage involves activities such as:
- Sending a welcome email with key information about the role and the facility. These include the start date, parking details, dress code requirements, a day one schedule and a contact person should they need additional information.
- Determining and assigning onboarding roles to ensure each employee knows what they're responsible for to ensure a smooth onboarding process
- Sending and completing pre-employment paperwork, such as tax and employment forms
- Preparing the workspace and IT resources the physician needs
Physician Orientation
The orientation process begins on day one and continues for several days, usually the first week after a physician begins working. The process includes:
- Clarifying their new role, responsibilities, performance expectations, and reporting duties
- Providing EHR training
- Providing training on mandatory compliance regulations, internal policies, and clinical best practices
- Reviewing the patients they will be seeing
- Providing a comprehensive facility tour and staff introduction
- An overview of the organization's mission, vision, core values, and workplace culture
- Meeting with the medical or clinical coordinator for the clinical ramp-up schedule and expectations
- Linking the new hire to a clinical quality coach to provide mentorship during the onboarding process.
- Provide a fully equipped workspace
Training
All physicians, regardless of education or experience, must go through training before they can start seeing patients when newly hired. This training includes compliance and role-specific training.
Compliance training is meant to introduce them to key regulations in the healthcare industry, such as HIPAA, the Anti-Kickback Statute, the False Claims Act, the Exclusion Statute, the Stark Law, the Civil Monetary Penalties Law, and OSHA.
Providing compliance training ensures your physicians know the legal, professional, and ethical standards of providing safe patient care.
Role-specific training tailored to primary care doctors equips new hires with the skills, knowledge, and competence to maintain patient safety.
Continuous Development
Supporting new physicians does not end with the first three months of employment. Instead, it transitions to ongoing support, where your facility continuously engages physicians and provides resources to support their professional development.
While physicians are responsible for their continuing medical education (CME), providing sustained support communicates to physicians that they are valued members of the organization and that you are invested in their growth. It also helps in maintenance of certification (MOC), keeping your practice compliant.
In addition to ongoing training, continuous development involves collecting regular feedback through:
- One-on-one check-ins with the supervising physicians to track employee progress, challenges, and areas where they need support
- Regular surveys to track the impact of the onboarding process and how the physician is adjusting to their new work environment
Once you've collected this feedback, you can identify actionable steps to take to ensure a smooth transition to practice for new physicians.
What Should be Included in a Physician Onboarding Checklist?
An onboarding checklist guides your onboarding approach by outlining the key steps before a new physician becomes a productive member of the organization. Developing a robust onboarding program starts with a checklist, which includes:
- All the key tasks involved in onboarding health care workers
- The departmental roles in onboarding, including the key staff responsible for each onboarding task
- The timelines for each onboarding activity. Many facilities adopt the 30-60-90-day template, but you can customize this based on your organization's needs
Here's a breakdown of onboarding tasks to include in your checklist:

How Can Technology and Software Improve Physician Onboarding?
Using onboarding software is the best way to streamline onboarding and get new physicians productive faster. Tools like ops.work streamline the process, reducing errors, improving consistency, and providing a positive experience for new hospital staff.
You can try our free plan to explore the various ways ops.work facilitates successful onboarding:
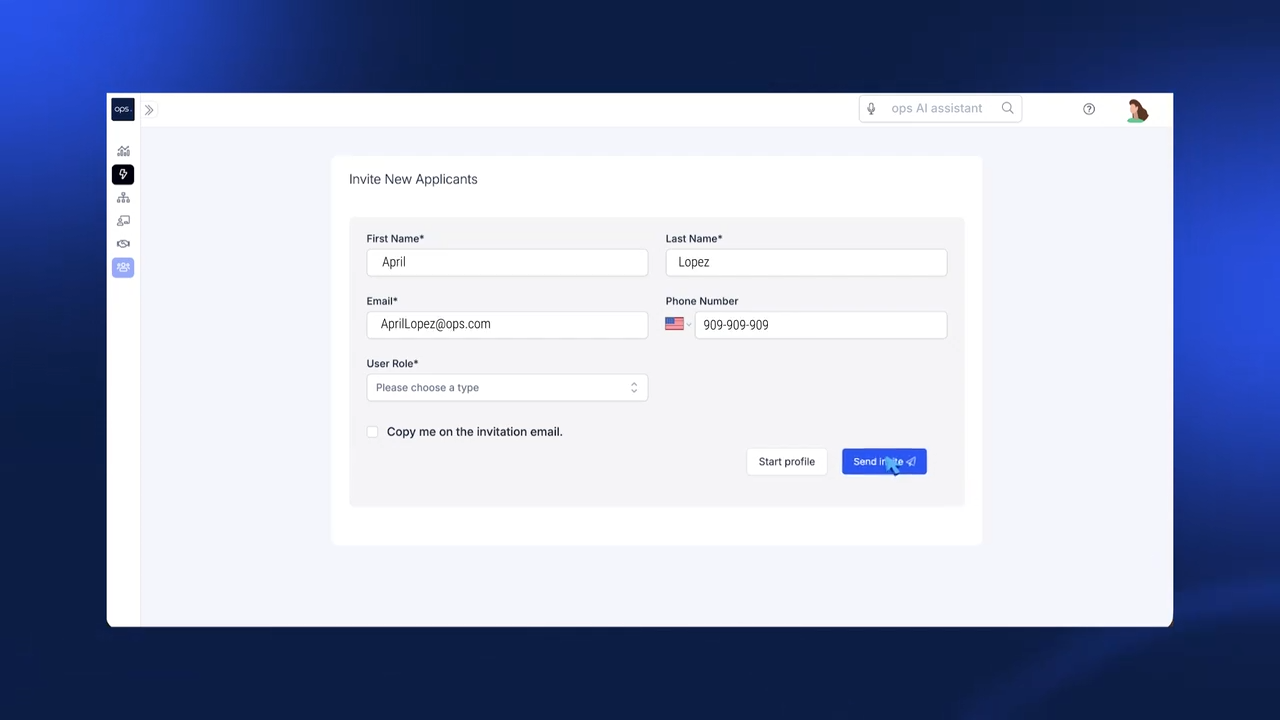
Invite new applicants onto your platform and create comprehensive employee profiles.
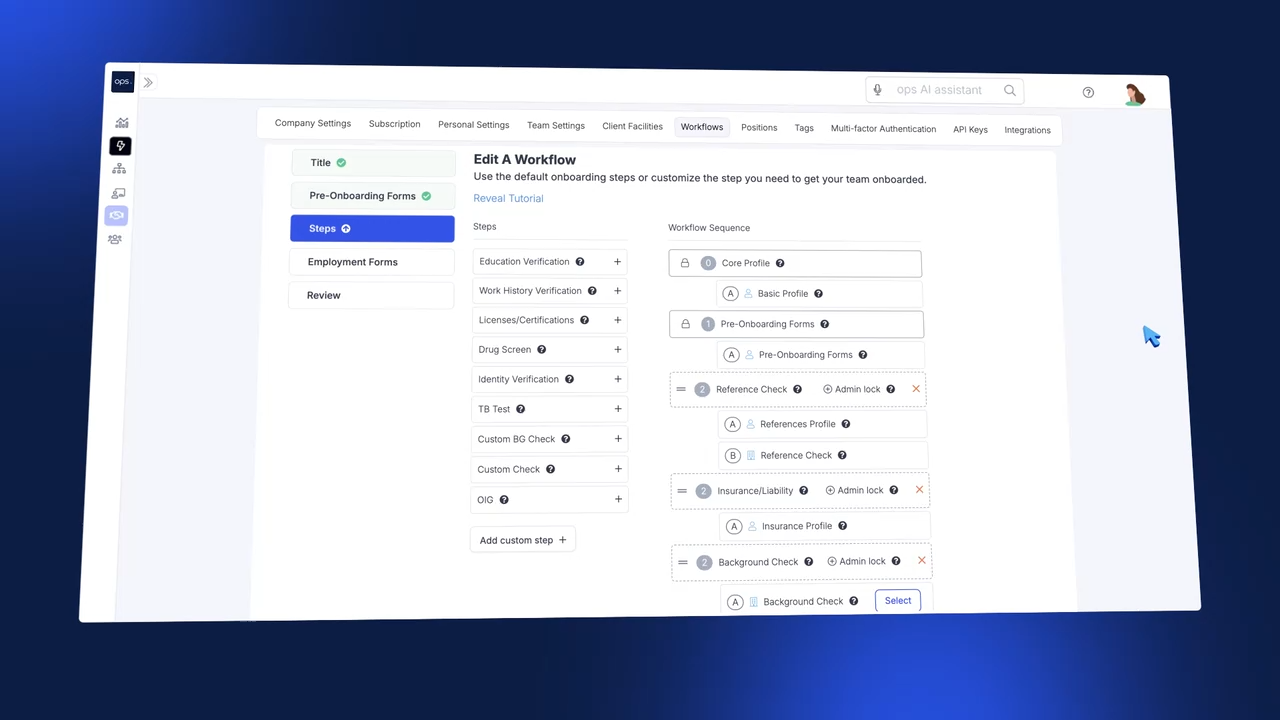
Create automated workflows to optimize manual processes such as credentialing and task management.
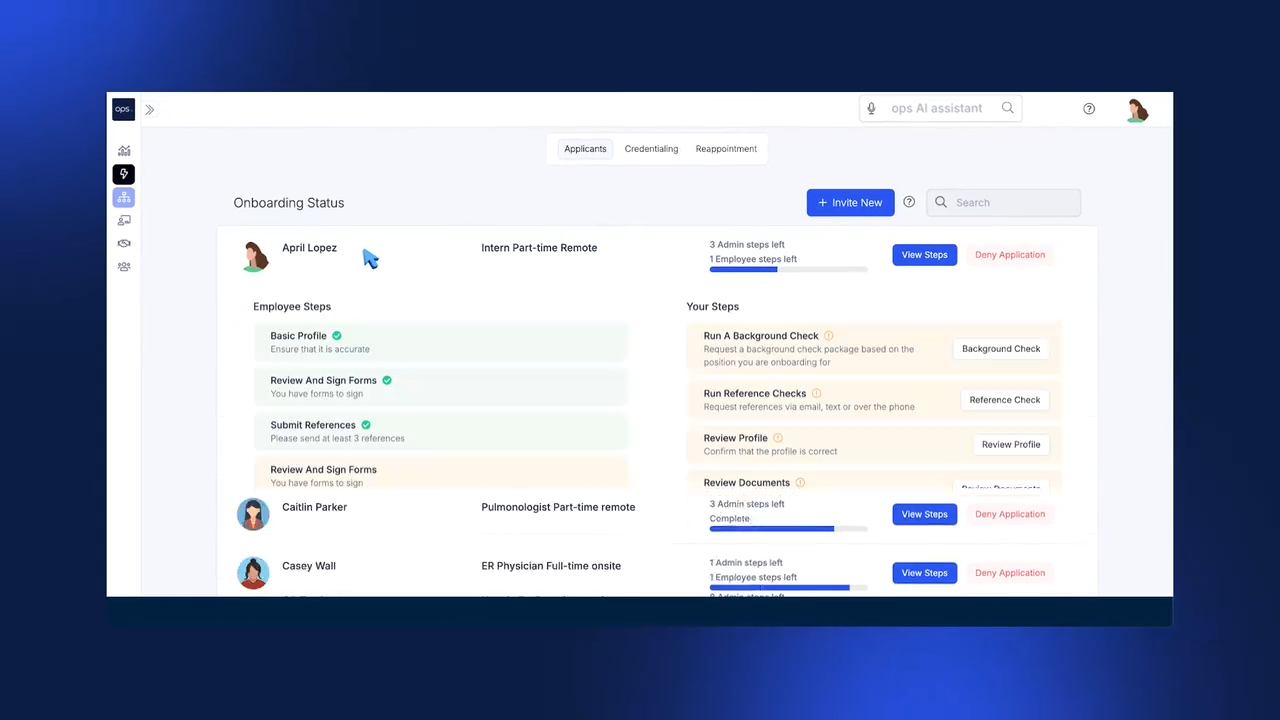
Track the progress of onboarding a new physician
Create comprehensive training modules to equip your care team with the technical and soft skills needed to succeed
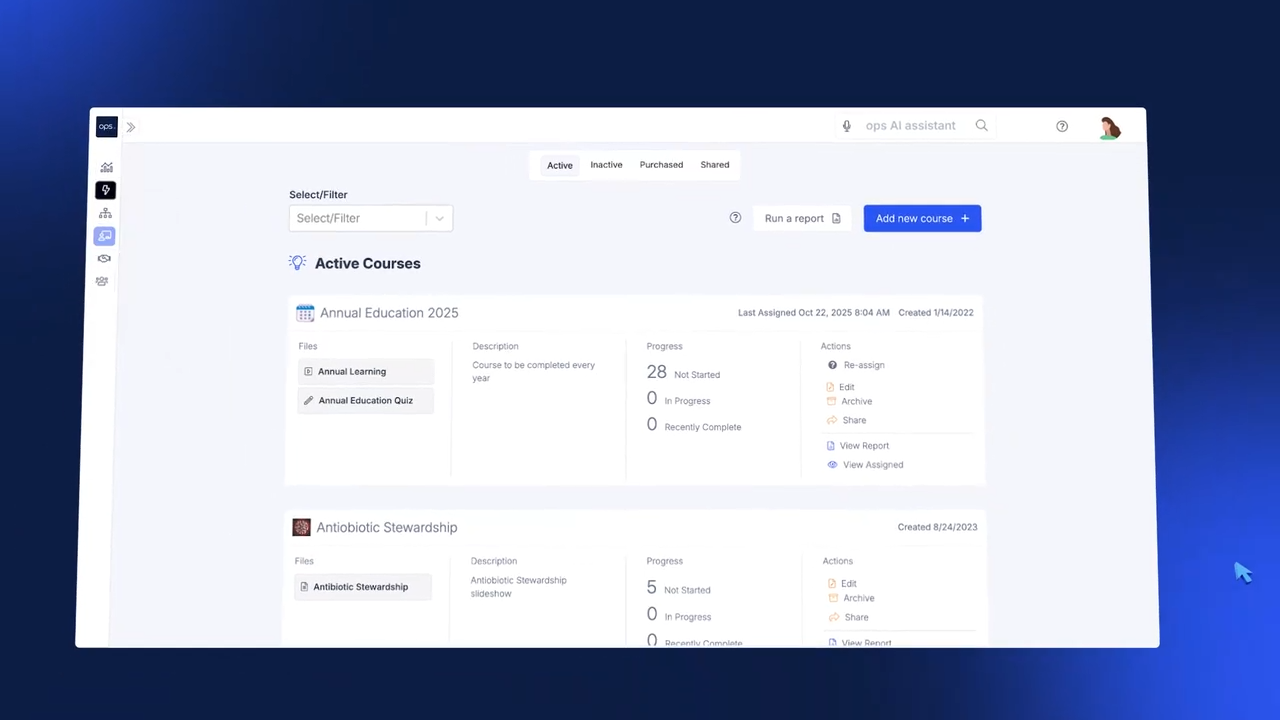
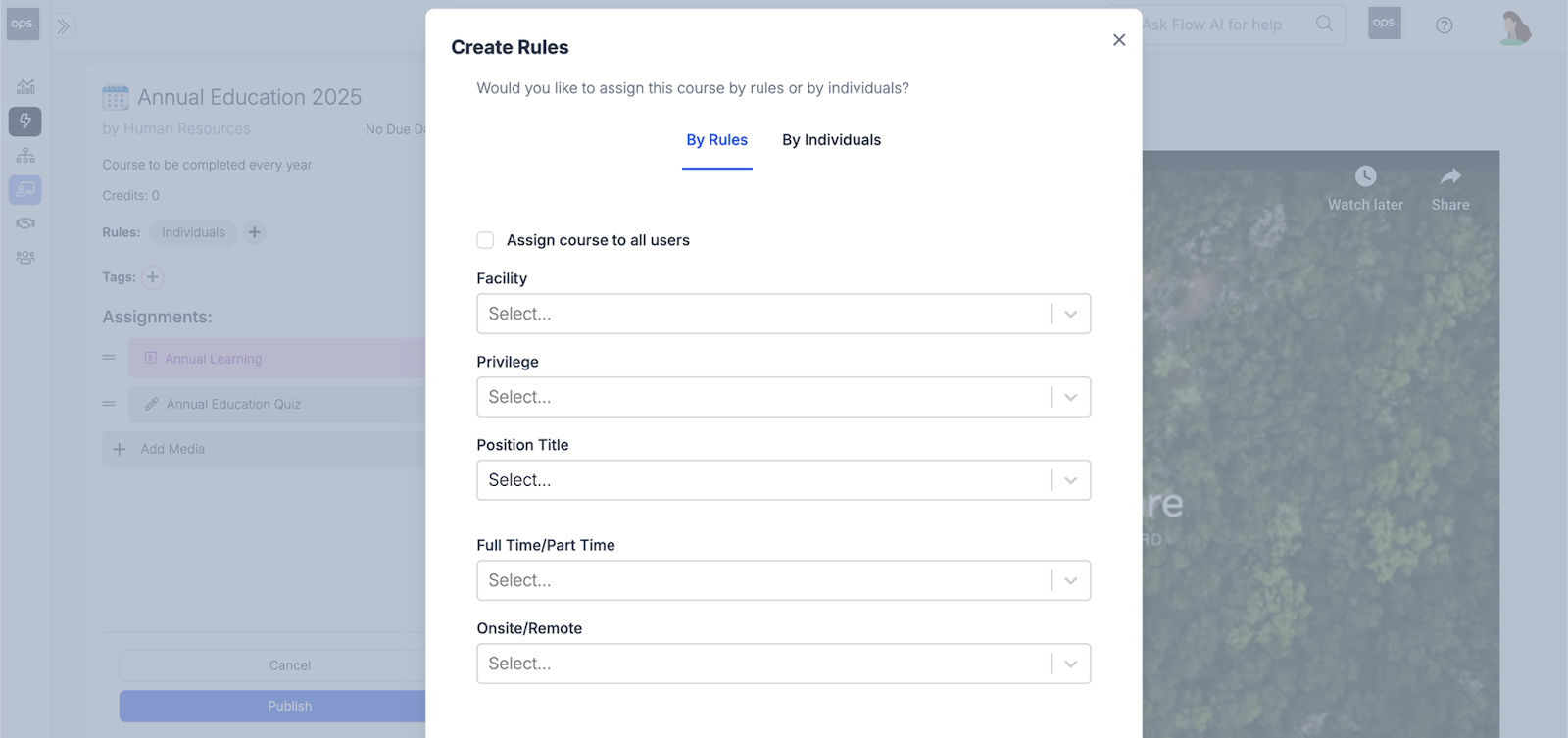
Assign specialty-specific training resources based on predetermined rules
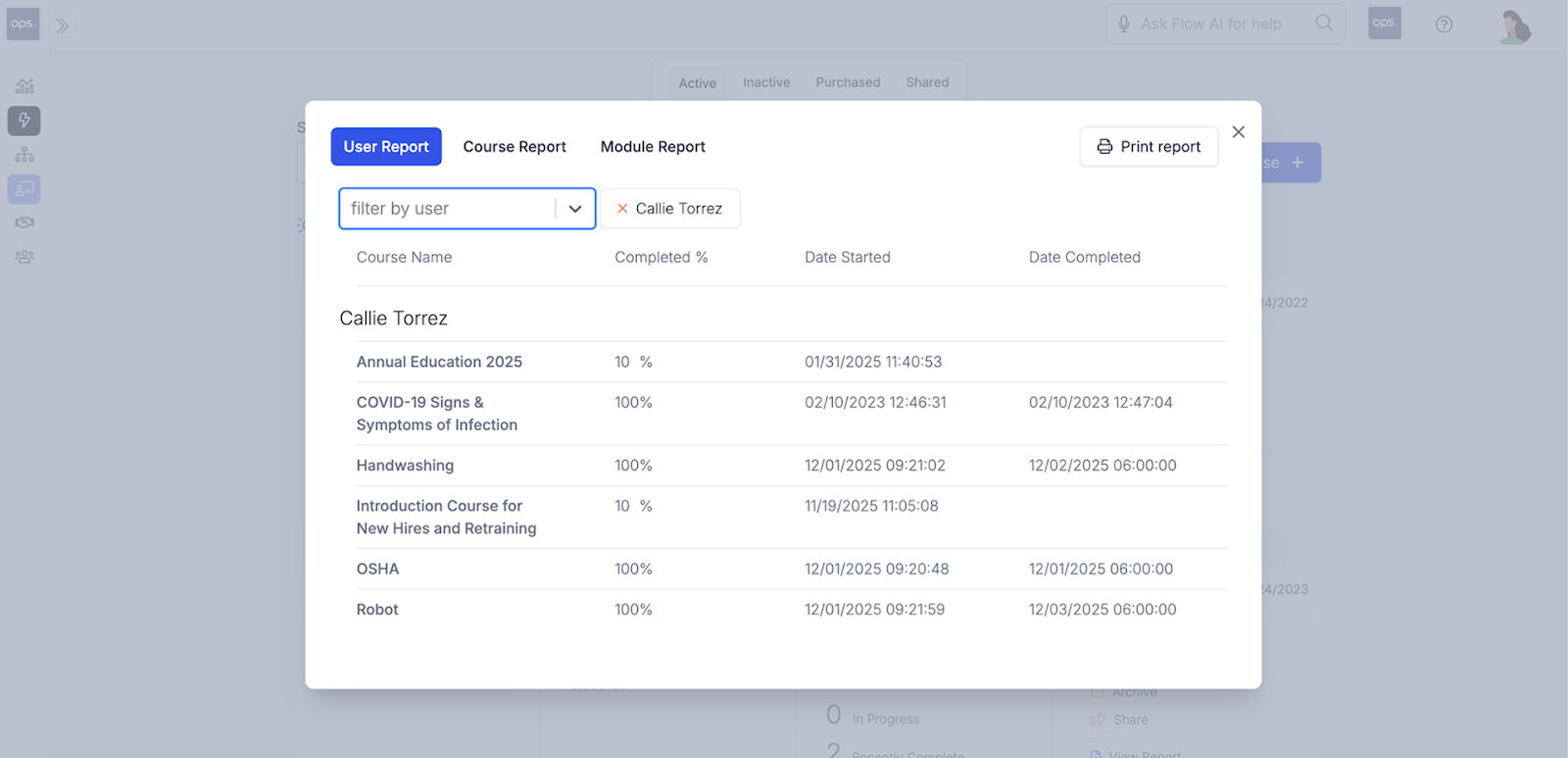
Generate LMS reports to gather insights on the impact of your training programs
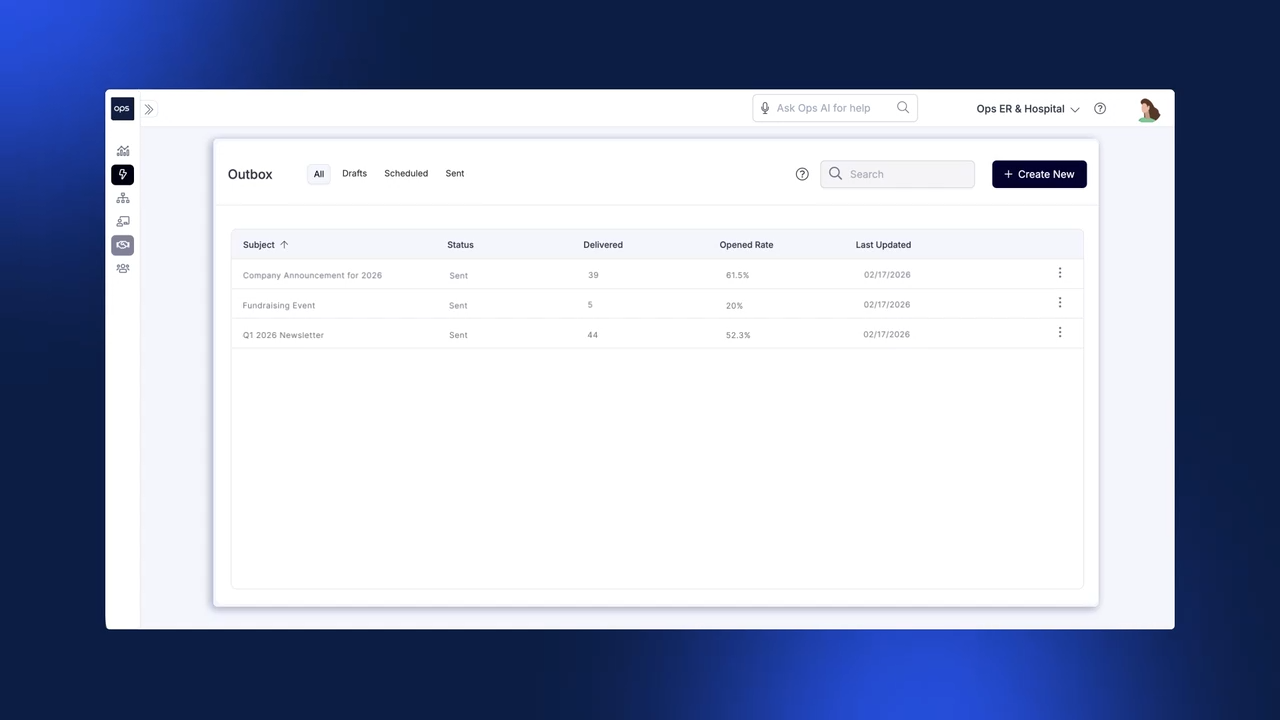
Send company-wide communication about your programs or other company resources
Create and send feedback collection tools to understand your employees' experience and track physician well-being
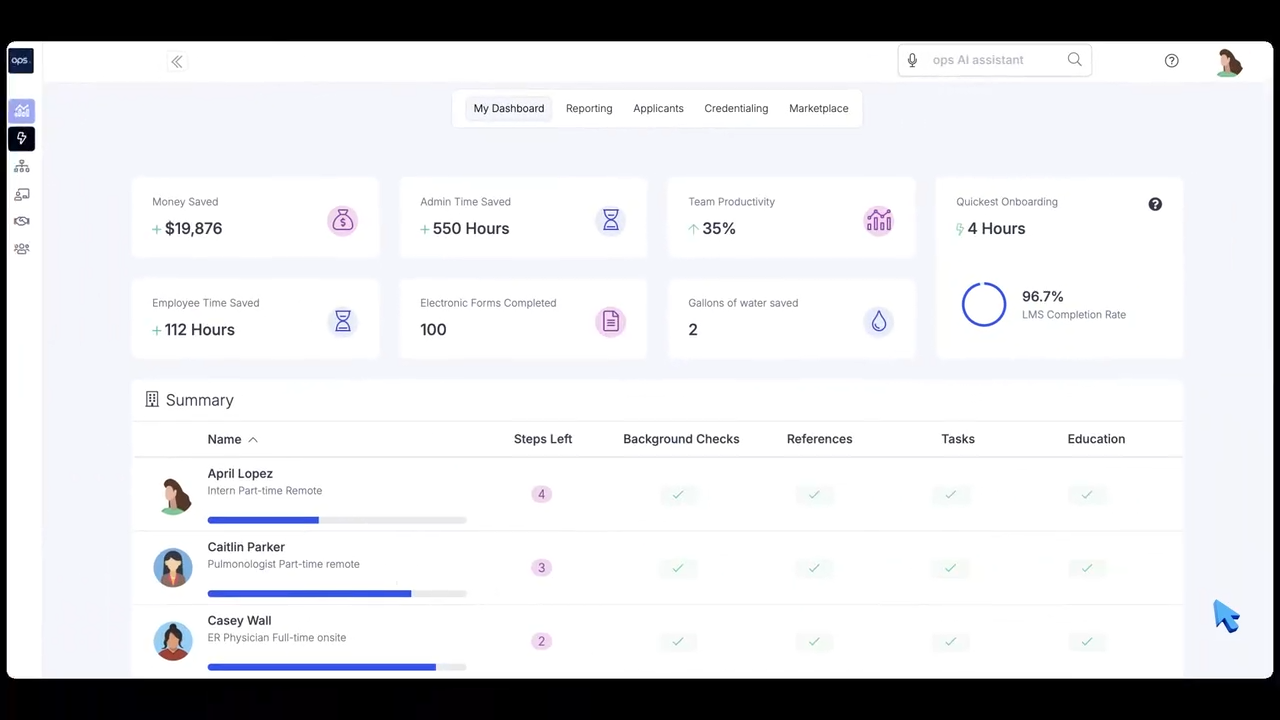
Track various metrics to measure the impact of your onboarding efforts on cost savings, training uptake, and ROI.
Conclusion
Retaining physicians and advanced practice providers is an ongoing concern for healthcare facilities. With rising turnover driven by burnout and disengagement, onboarding helps keep new physicians engaged and productive. It allows you to provide them with the necessary tools and resources as you gradually increase the patient volume throughout their first year of practice. Tools like ops.work streamline onboarding, resulting in maximum efficiency and cost savings. Get started with our free plan to improve how you integrate new employees into your primary care practice.
References
Jimenez, Geronimo, et al. “Revisiting the Four Core Functions (4Cs) of Primary Care: Operational Definitions and Complexities.” Primary Health Care Research & Development, vol. 22, no. 1, 10 Nov. 2021, p. e68, www.ncbi.nlm.nih.gov/pmc/articles/PMC8581591/, https://doi.org/10.1017/S1463423621000669.
Patel, Roshan , and Sandeep Sharma. “Credentialing.” Nih.gov, StatPearls Publishing, 24 Oct. 2022, www.ncbi.nlm.nih.gov/books/NBK519504/.
Peck, C. “Continuing Medical Education and Continuing Professional Development: International Comparisons.” BMJ, vol. 320, no. 7232, 12 Feb. 2000, pp. 432–435, https://doi.org/10.1136/bmj.320.7232.432.
Frequently Asked Questions
- First contact
- Comprehensiveness
- Coordination
- Continuity
An effective onboarding program includes five key components: compliance, culture, connection, confidence, and clarity. Combined, these elements ensure a positive onboarding experience for new physicians.
Onboarding teams consisting of human resources, practice managers, medical staff offices, IT, L&D teams, and an onboarding coordinator facilitate physician onboarding.
The formal onboarding process lasts a minimum of three months but can continue for up to the first year of practice, depending on the facility and its needs.
Common challenges when onboarding physicians include starting the credentialing process too late, unclear job descriptions and performance expectations, and overreliance on manual processes.